Insights
Learn tips and current trends from the experts on workplace health, wellness and safety. Subscribe to our Insights blog today.
Recent Posts
Filters
-
 Posted
PostedMay 6, 2024 in ConstructionOnsite Medical As a Tool for Attracting and Retaining Skilled Construction WorkersRead Article -
 Posted
PostedApril 29, 2024 in Onsite CareFuture Trends in Onsite Health Clinics: Embracing Technology and InnovationRead Article -
 Posted
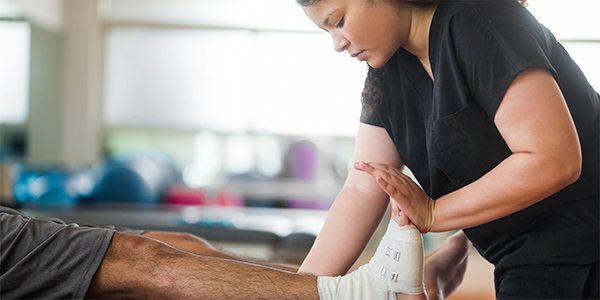
PostedApril 22, 2024 in Onsite CareHow Onsite Physical and Occupational Therapists Help Your WorkersRead Article -
 Posted
PostedApril 15, 2024 in Onsite CareHow Onsite Care Provides Better Outcomes for Employers and EmployeesRead Article -
 Posted
PostedApril 8, 2024 in TelehealthHow Teletriage Improves Patient Access to CareRead Article -
 Posted
PostedApril 1, 2024 in Occupational Health10 Questions to Ask Before Choosing an Occupational Health ProviderRead Article -
 Posted
PostedMarch 25, 2024 in Onsite Care5 Ways an Onsite Clinic Can Help You Hyper-Personalize Your WorkplaceRead Article -
 Posted
PostedMarch 18, 2024 in ConstructionBuilding a Strong Foundation: Prioritizing Mental Health in ConstructionRead Article -
 Posted
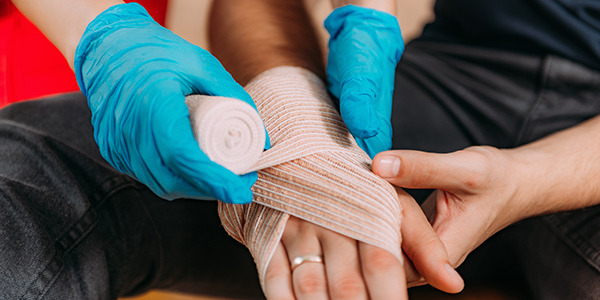
PostedMarch 11, 2024 in Occupational HealthTime of Need: Benefits of First Aid in the WorkplaceRead Article -
 Posted
PostedMarch 4, 2024 in Employee Wellbeing3 Benefits of Health and Wellness Programs in the WorkplaceRead Article -
 Posted
PostedFebruary 26, 2024 in Onsite CareDrug Screening and Workers’ Compensation: Understanding the LinkRead Article -
 Posted
PostedFebruary 19, 2024 in Occupational HealthHow to Start Your Occupational Health ClinicRead Article
1
Posted 1
1
View Page