Fixed-Location Onsite Clinics
Permanent Health Centers Designed Around Your Workforce
Medcor’s fixed-location onsite clinics put high-quality occupational healthcare right where your employees need it most: at work. By integrating clinical care directly into your facility, we help employers reduce recordables, lower costs and keep teams healthy, productive and safe.
Looking for a different clinic model?

Care That’s Close, Consistent and Cost-Effective
Our onsite health centers operate as an extension of your organization, staffed by Medcor Advocates who understand the unique risks and needs of your workplace. With evidence-based protocols and streamlined technology, every visit delivers consistent, compliant care, from injury triage to wellness support.
Benefits include:
- Immediate treatment for work-related injuries and illnesses
- Fewer ER visits and lower workers’ compensation costs
- Faster return-to-work outcomes and better productivity
- Improved OSHA and regulatory compliance
- Enhanced employee satisfaction and retention

Tailored to Your Worksite
Every Medcor clinic is designed around your environment, workforce and operational needs. Whether embedded in a manufacturing facility, distribution hub or complex construction site, our clinics deliver the right level of care where it’s needed most.
- Injury and illness care
- Medical surveillance and screening
- Audiometric Testing and Employee Screening Services
- Preventive health education and wellness initiatives
- Case management and follow-up care
Our fixed-location models are scalable and customizable, ensuring you get exactly the level of service your organization requires.
Why Employers Choose Medcor

-
40+ years delivering occupational health solutions across North America.
-
Continuous quality monitoring by Medcor’s Clinical Affairs team.
-
Proprietary EHR and reporting tools for transparency and insight.
-
Proven ROI through fewer claims and improved workforce health.
How Onsite Clinics Increase Quality of Care
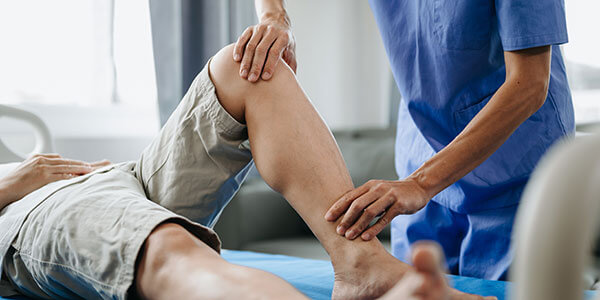
Bringing Medcor onsite to your workplace with an employee clinic means employees have an advocate who can help them with work-related injuries, preventative screenings, urgent care conditions, testing, return-to-work programs, preventative medicine, health coaching and more.
Because we are onsite, our early intervention means that health concerns are addressed before a claim can happen. When referrals are necessary, Medcor navigates patients through provider selection and the traditional healthcare system to ensure optimal health outcomes and the most cost savings. This convenient access to care ensures employee health is maintained, boosting productivity and reducing wait times for treatment.
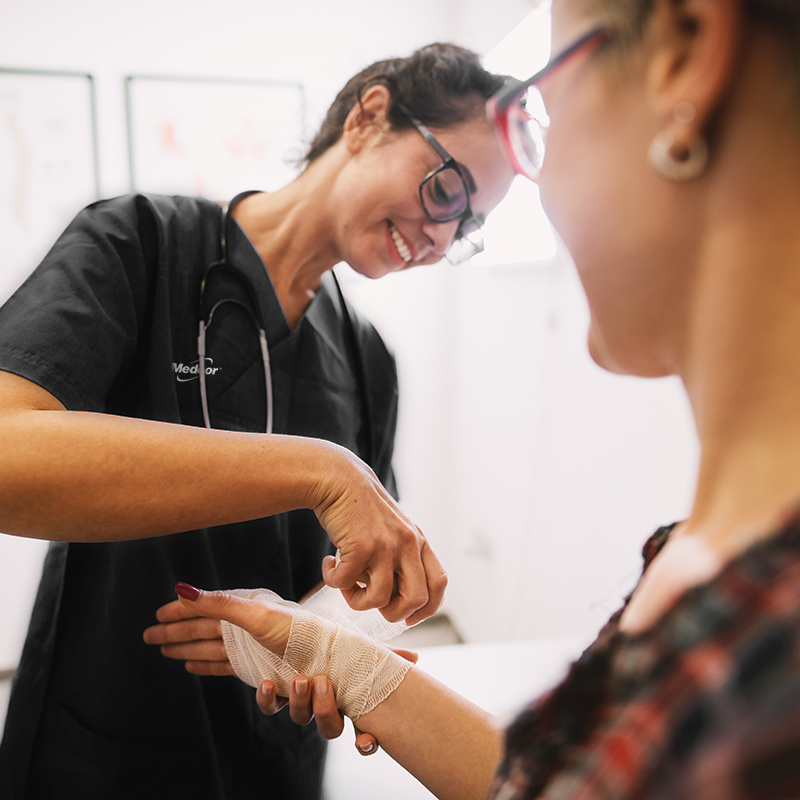
Why Flexible Employee Health Programs Matter
In today’s fast-changing business environment, supporting employee wellbeing is key to maintaining a competitive edge. Flexible health programs allow businesses to adapt to shifting workforce needs, improving satisfaction, reducing costs and promoting long-term wellness.
Adapt to Changing Needs
As business priorities and employee demographics shift, flexible health programs allow companies to adjust benefits—whether adding mental health support or introducing telehealth services—ensuring employees get the right care at the right time.
Boost Employee Satisfaction
When employees see that their health needs are valued, engagement and retention improve. Tailored benefits like wellness workshops and stress management resources foster a healthier, more committed workforce.
Control Costs
Customizable health programs prevent overspending on unused services, directing resources to where they have the most impact—improving care quality while lowering costs.
Support Long-Term Wellness
Proactive, flexible health solutions help prevent future issues and create a healthier, more resilient workforce, strengthening employee loyalty and business performance.
Benefits of Onsite Clinics
Onsite health clinics provide your employees with convenient access to medical care for injuries and essential care services. For some workers, having convenient access is the difference between receiving routine care such as preventative screenings, injury and illness treatment and wellness services and delaying medical care. You benefit from a healthier workforce and increased productivity when your employees have easy access to care. By focusing on worksite health and offering comprehensive care, you ensure the long-term wellbeing of your employees.
- Encourage a Healthy Workforce
- Reduce Risks
- Prevent Unnecessary Claims
- Facilitate a Safe Return to Work
- Increase In-Network Provider Utilization
- Provide Care Consistency
Frequently Asked Questions
-
You do. Medcor operates as a steward of your space and equipment. You own the physical assets; Medcor provides the staffing, clinical protocols, technology and day-to-day management.
-
Staffing is configured to your scope of care. Depending on your needs, a fixed-location clinic can include Worksite Health Technicians (EMTs/paramedics), Athletic Trainers, LPNs/LVNs, RNs, Social Workers, NPs, PAs, physicians and Mental Health Specialists. Medcor works with you to match staffing to your workforce and clinical requirements.
-
Yes. Medcor provides pricing transparency for clinic build-out and ongoing operations, including a range for simple first aid rooms through larger advanced care facilities. We can also help you assess your current healthcare spend, including costs absorbed through insurance and offsite care — so you have a clear picture before making a decision.
-
For essential care clinics, implementation typically takes 90 days from contract execution to go-live. Advanced care clinics require approximately 120 days, reflecting the additional credentialing, physician oversight structures and clinical configuration involved. Medcor guides you through the full process.
-
Hours are client-configured. Clinics can operate during a single shift, expanded hours covering early morning or evening, or around the clock with 24/7 coverage — depending on your workforce’s needs and your operational requirements.
-
Beyond episodic injury and illness care, fixed-location clinics can include medical surveillance and screenings, audiometric testing, physical therapy, athletic training and ergonomic assessment, health coaching, mental wellness support, immunizations, chronic disease management and advanced care services including routine physicals. Scope is client-configured.
-
Medcor’s Clinical Affairs team provides continuous oversight through proprietary quality monitoring systems. The Proactive Program Management (PPM) platform gives real-time visibility into clinic operations, clinical quality indicators and performance metrics across all locations, enabling early identification of issues and consistent standards.
-
The difference is usually in the systems behind the care. Medcor brings standardized clinical protocols, proprietary EMR and reporting technology, OSHA recordkeeping integration and a dedicated quality assurance process, things most in-house or single-provider models lack. Clients who switch typically see improvement in recordable rates, reporting consistency and employee satisfaction scores.